A lot of rib pain is thought to be caused by dysfunction in the upper back (thoracic spine) and the surrounding muscles. There is evidence available which supports treatments in this area which are likely to have a knock-on effect on the rib pain.
Symptoms:
-
Pain under the ribs.
-
Pain over the breast-bone (sternum).
-
Pain between the ribs at the front or at the back (between the shoulder blades).
-
Pain when taking a deep breath.
-
Pain when twisting (especially if repetitive).
-
Pain when stretching over to the sides (especially with a twist).
Causes:
-
Babies kicks!
-
Bigger uterus / growing baby – adding pressure to the internal organs and ribs.
-
Changes in hormones allows the increased movements of joints, this can include the joints of the rib cage.
-
Stiffness in the upper back or postural changes from the growing baby can put added pressure on the rib cage.
-
Growing breasts – increased weight on the chest may weigh heavy on the upper back and contribute to a change in posture and pressure on the rib cage.
-
Tension / stress – can increase tension in muscles that attach to the ribs and pull on the joints and ligaments.
-
The growth and movement of the baby also put pressure on your diaphragm, causing that well known feeling of breathlessness with little exertion. This extra pressure can also irritate the nerves in the diaphragm and make you more sensitive to pains around the ribs and shoulders.
Here is what the evidence says about the treatment options:
Exercise – There are so many benefits to staying active during your pregnancy. If upper back or rib pain is getting in your way then try some stretches daily like these from our friends at Kerry Physiotherapy.
Yoga – Yoga has been studied for it’s many benefits. THIS study showed benefits for the upper back when doing just 10 mins of yoga a day for 1 month. It also showed that doing this helped improve the participants mood.
There are lots of Online Yoga programmes available, have a look at our Top 5 here (and why we love them)! You can also read our blog on how yoga can help in other ways.

Pilates – Pilates‐based thoracic exercise could increase thoracic extension and side‐bending mobility, and thus, contribute to the improvement of disability and function in patients with upper back and neck pain according to this study. Another study looked at the overall effects of Pilates on pregnancy and the birth and concluded that a physical activity programme of 8 weeks, based on the Pilates method, improves functional parameters in pregnant women and benefits delivery.
Have a look at our Top 5 online Pilates options here.
Kinesio Tape – We have looked at evidence surrounding Kinesio-tape and it suggests that the use of Kinesio-tape can be really helpful with upper back pain, especially if it is affecting the upper trapezius region (upper shoulders, next to the neck). The study also shows that if you combine kinesio-taping with strength work like Pilates programmes then you get an even greater decrease in pain and improved range of movement.
This is the tape that we recommend based on our own use and reviews and HERE is a really short video showing an easy application method for the tape.
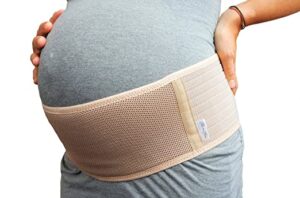
Pregnancy support belt – Support belts can help to take some of the pressure from the growing bump. They also support the back and pelvis which can help improve posture and relieve pressure on the ribs. There is little research behind the use of maternity belts when it comes to rib pain but they are certainly worth a try.
Here are our Top 5 maternity belt options.
Trigger point release – Trigger point release is the hold of pressure over points (knots) in muscles that temporarily stops blood flow, this makes the contraction relax and also then increases blood flow to the muscle once released. Evidence shows that dry needling and trigger point release is effective in treating upper back and neck pains. THIS study shows that both dry needling and manual trigger point relief have positive results when treating upper back and neck pain and that neither technique is superior to the other. Dry needling would involve booking in with your local Physiotherapist (who is a registered acupuncturist).
Carrying out your own trigger point release can be easily done using a specific ball like this one (which we recommend based on it’s 3000+ reviews).
Trigger point release helps to relieve the tension in the muscles around the affected areas, it can give an almost instant result. Check out this video for a great ‘how to’ guide.
Symptoms to watch out for:
some of the symptoms mentioned above might be associated with pre-eclampsia. In its early stages pre-eclampsia might present as:
-
high blood pressure noted at your midwife / GP appointment.
-
protein in urine at your usual midwife check-ups.
It is therefore essential that you keep up to date with all of your prenatal appointments.
Further symptoms might include:
-
Severe headaches.
-
Vision problems, such as blurring or seeing flashing lights.
-
Pain just below the ribs.
-
Vomiting.
-
Sudden swelling of the feet, ankles, face and hands.
-
Weight loss
-
Severe night pain
-
Fever / chills